UND microbiologist: Coronavirus solution will take time
Nadeem Khan on the front lines looks for links between flu and COVID-19 viruses
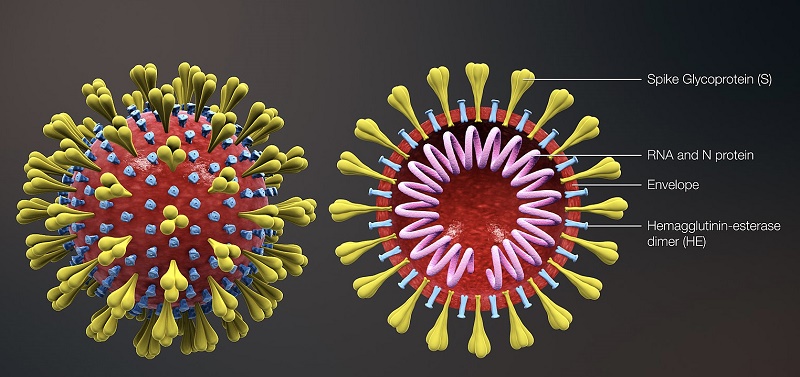
As scientists around the world seek solutions to the worldwide coronavirus (COVID-1) pandemic, Nadeem Khan views his influenza research at the University of North Dakota as a potential important link in understanding the similarities and differences between COVID-19 and seasonal flu.
“What we are studying is the synergism between the flu virus and respiratory bacteria and how flu helps these bacteria to cause disease of varying severity,” said Nadeem Khan, an assistant professor in the UND School of Medicine & Health Sciences. “Understanding this should help us to develop better vaccines. We should be able to intervene in a more targeted, better way so that we are able to contain flu-induced bacterial disease.”
Khan holds Ph.D. degrees in microbiology and immunology. He was a postdoctoral fellow at Rochester General Hospital in Rochester, N.Y., and at the Albert Einstein College of Medicine in New York City, where he spent several years studying influenza and influenza-associated pneumonia.
In 2017, he accepted a faculty research position at UND to investigate influenza, flu-associated bacterial pneumonia, how it manifests into disease and how to better contain and treat it. Khan’s lab recently received a five-year, nearly $2 million grant from the National Institutes of Health (NIH) for flu-related research.
Researching connections
By next month, Khan expects his lab to be working on some aspect of the coronavirus using non-infectious particles and components. He believes it’s possible that the flu and COVID-19 viruses are operating through the same disease-causing mechanism in the body.
“The difference could be that COVID-19 might be slightly more intense in terms of causing disease,” Khan explained. “If you find that, it’s significant because what we’re studying with the flu could be extrapolated to COVID-19. We contemplate establishing a bridge that takes our flu-specific investigation to include the COVID-19 system.”
Khan visited with UND Today about how his research at UND relates to the COVID-19 pandemic. The following Q&A has been lightly edited for clarity.

How would you describe the primary focus of your research?
There are two different aspects of influenza disease. The first aspect is how the influenza virus causes disease. It can cause disease with mild symptoms of sore throat, sinus infection and pneumonia. In the worst-case scenario, the pneumonia can turn fatal, although that happens rarely. Once you completely understand the process and the mechanisms of influenza-mediated disease pathogenesis, you are not only able to control the disease, but you’re also then able to design better vaccines that are more effective than those currently on the market. Our central focus is to better understand pathogenesis – the progress of disease – of flu in the respiratory system.
What’s the difference between COVID-19 and seasonal flu?
The fundamental difference with the flu and the COVID-19 situation we have right now is that there are two kinds of flu: the pandemic flu – which we have seen three or four times over the past 100 years – and the seasonal flu that can infect you with different types of influenza strains almost every year.
Let’s say we both took the same flu vaccine, but I travel to a coastal state while you stay in North Dakota. You get infected with a strain you’re protected against. I get exposed to a strain that was not part of the vaccine I took, and I’m not protected. Therefore, in the case of seasonal flu, you could be infected with multiple different kinds of viral strains, which is why we don’t have a vaccine with similar or equal efficacy. In some people, the efficacy of the seasonal flu vaccine could be as high as 60 percent. In other people, the efficacy could be as low as 10 percent because of the diversity of flu strains in the circulation. In a COVID-19 situation, you are being infected with only one virus, SARS-CoV2.
What happens in the case of flu vaccines is that in the best-case scenario, you are protected. The worst-case scenario is that you’re exposed to a new strain which wasn’t in the vaccine. Your vaccination could still provide you with a bit of cross reactivity. It could still work to reduce the severity of the infection you would otherwise develop. That’s the data we have.
So when you came back to North Dakota, you could infect people, even if they had the flu vaccine?
That’s how the strains evolve. For instance, if I’m well-protected against the virus strains in North Dakota, I’m fine as long as I’m not traveling out of the state. If I’m traveling, I can get infected with a new strain, bring back that strain and transmit it into the community.
Do we have a good understanding of how the coronavirus works?
We have a good understanding of this virus, but not a complete understanding because it’s still evolving. What we know right now is that in many ways, COVID-19 could present the symptoms in a very similar manner to the flu. Oftentimes, you’ll have symptoms that are typical of flu, and you can’t tell whether it’s the flu or COVID-19.
The ideal scenario would be that if you had symptoms – a cough, sneezing, a fever or body aches – it’s time to go seek help and get tested. The difference is that with flu, you need direct contact with a person to transmit the infection. With COVID-19, direct contact isn’t necessary. If a person with COVID-19 sneezes or coughs into the air, the virus has the ability to hang around in the air or stay on surfaces, and then infect someone. It might take four to 10 days to present the symptoms. During this period, if you are a carrier of the virus, you might not have active symptoms, but you’re still transmitting the virus to the community.
Is it a matter of collecting more data?
That’s right. Understanding the COVID-19 epidemiology and the ability of the virus to transmit will only be possible with the collection of data over time, but we have a good understanding of the data in the public domain. We know that social isolation is definitely needed to contain the transmission.
With the coronavirus outbreak, what should be the top priority?
We can’t be running after a vaccine at this point because developing a vaccine is a complex scientific process. It goes through various phases, starting in the laboratory, through quality control and many other complex steps. It may not happen in a year or a year and a half. We may never have an effective vaccine against COVID-19 because we haven’t yet developed one for the flu. Our priority is to contain the transmission of this virus so that we can minimize the risk to the community as much as possible. It is likely that by the time we have the vaccine, the virus is no longer in circulation in the community, and we never get infected with the virus again. Right now, the immediate priority is to contain this virus as much as possible so that we don’t overwhelm our health care system.
Is one of the worst things you can do is act as if this coronavirus pandemic doesn’t matter?
Absolutely. If you are immune competent – if your immune system is fine – and you’re not old, chances are that you will be fine. But by protecting yourself, you are indirectly protecting somebody who is at risk. Whether you interact with several or tens of people every day, you don’t know who is and who isn’t at risk. If you carry the virus and you’re 35 or 40 years old, it will give you some symptoms and you could be transmitting it to somebody who’s potentially at risk. This is the circle that’s connecting everybody. By containing yourself, you are helping protect the people at risk. Suppose tomorrow, you meet somebody who had a kidney transplant or is having cancer treatment. They could be on an immune-suppression treatment, so their immune system is down. They are at increased risk, and it has nothing to do with age.
Are you optimistic that people are beginning to understand this outbreak and how they should react to it?
I think what happened it Italy was a wake-up call. It sends a message around the world that the best way to contain this virus is to do a social isolation, as much as we can, for two to four weeks. If we do that consistently, I’m sure we’ll contain the virus. At the moment, it’s the best option and best way forward. People are increasingly learning this, accepting that it is a problem, and this is how we must tackle it. We are putting the effort into doing it.
Do you envision a time when we’ll be able to better predict what type of vaccine we’ll need heading into the flu season?
Currently, the situation is that we have two significant vaccines on the market that everybody should be vaccinated with. The first vaccine is the flu vaccine that all of us should be taking and the second vaccine is the pneumococcal vaccine, known as the pneumonia vaccine. Although they have nothing to do with the COVID-19, they are vaccines that can give you significantly better immunity to fight flu and flu-associated bacterial pneumonia. Certainly, we want to develop a vaccine for COVID-19, but we don’t yet know whether new strains will emerge or how well they will cross-react. That is something we will only learn with time. There are no easy answers.



