O Pioneers!
UND’s trailblazing Department of Physician Assistant Studies celebrates 50 years of improving access to health care in rural communities
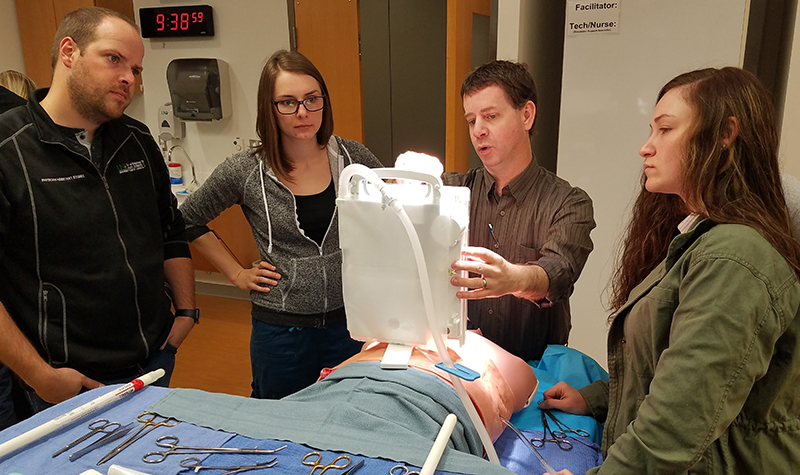
“I was out at Cass Lake [Minnesota] a while ago and fell and lacerated my arm,” recalled Dr. Robert Eelkema. “We went to the Cass Lake clinic, and one of our graduates was there and sewed me up. I felt pretty good about that.”
Speaking of a graduate of the Physician Assistant Studies program at UND’s School of Medicine & Health Sciences, the nearly 90-year-old Eelkema recalled the anecdote with an almost palpable pride.
And proud he has every right to be: this physician assistant, or PA, in rural Minnesota was the product of a program Eelkema had himself brought to North Dakota five decades ago on little more than grit and gumption.
“Our goal was to get people out to provide health care in the boonies quickly,” Eelkema continued of the highly innovative program dedicated to producing providers focused almost exclusively on rural communities. “We wanted the best way of doing it and wanted to get them employed right at the start, sort of like a deployment strategy.”
And so was born in 1970 the program — the Medical Extension or “MedEx” program — that would become the SMHS Department of Physicians Assistant Studies, which celebrates its 50th birthday this year.
Ex Nihilo (‘out of nothing’)
“Deployment” is the perfect word to use here.

As Eelkema put it, in the late 1960s and early 1970s, many corpsmen with a glut of trauma and other medical experience — but no medical degree — were returning from Vietnam and looking for work. Many of these former medics were interested in health careers, but not necessarily medical school.
And given the fact that this was an era before the “paramedic” was a career option in many states and nurses were still overwhelmingly female, a new profession had to be invented to accommodate the skills and experience of these veterans.
So Eelkema and his allies did just that, almost out of nothing.
“He’s a North Dakota original,” noted one of those allies — Dr. Jim Brosseau, who in the 1990s oversaw the program when it was housed in what used to be called UND’s Department of Community Medicine. Like Brosseau, Eelkema had grown up in Drayton, N.D., and shared his friend’s passion for rural health. “Bob had a real knack for writing federal grant proposals and getting them funded. He was truly a ‘founder’ of today’s School of Medicine & Health Sciences.”
At a meeting of the American Public Health Association in Philadelphia in 1969, the newly appointed chair of what is now the Department of Family & Community Medicine bumped into a former colleague named Richard Smith.
“He’d just got back from Africa with the Peace Corps,” Eelkelma recalled over the phone. “I asked him what he was doing now, and he said, ‘I’m working with MedEx.’ “I said, ‘What’s MedEx?’ and he gave me his card and said, ‘Call me.’ So I did. He was working to repatriate independent duty corpsman into health care. At the time, there was only one other program that was training these guys, and that was Duke University.”
The pioneering state of North Dakota was next.
According to Eelkema, after chatting with Smith and meeting with some well-placed officials in Washington, including Dr. Paul Sanazaro, director of the National Institutes of Health’s Department of Health Manpower Research, the SMHS received a $1.7 million federal grant to train former medics — and eventually nurses — for general health practice in rural areas.

As Eelkema, Patrick McGuire and former UND President Tom Clifford recounted those early days in their 2004 book Good Medicine, Eelkema had won the grant despite the fact that the paperwork making Eelkema’s hire official had been delayed by former SMHS Dean Ted Harwood.
“Though he’d been operating as chair of the department for some months, officially Eelkema didn’t exist,” the trio of authors wrote. “And so it was that [former UND President George] Starcher had to go before the State Board of Higher Education and ask permission to officially hire the man who had just landed the [at the time] largest grant in the history of the state.”
But as the number of returning soldiers dwindled, the MedEx program, which was housed in Eelkema’s department, turned to the UND College of Nursing & Professional Disciplines (CNPD) for support. And after only a few years, MedEx came to rely almost exclusively on nurse applicants in the years before the family nurse practitioner (FNP) was a formal category.
“[Veterans] weren’t applying anymore,” Eelkema continued, referencing with gratitude the assistance he received from his nurse-colleague Mickey Knutson. “It worked better with nurses anyway since a lot of the former medics came from Chicago or other large cities, and were less happy to be in rural areas.”
So the program evolved into a “dual accreditation” program to produce both nurse practitioners and what were by now being called physician assistants. The program held this dual accreditation status from 1976 to 1992, at which time the FNP component of the program was transferred fully to the nursing college.
“When I left the university in 2000, we’d trained 1,100 physician extenders,” concluded Eelkema. “We were training PAs who had been nurses. They’re good. The UND nursing school is a good group; I have a lot of respect for them.”
The Student Becomes the Master
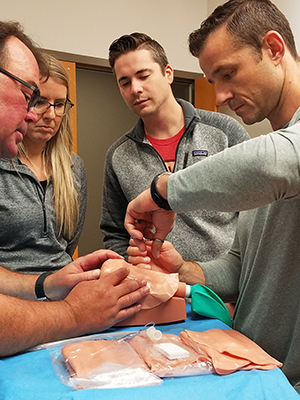
The program turned to one of those nurses to help it take the next step around the turn of the century.
“I’m a graduate of that program in dual certification,” beamed Mary Ann Laxen, one of the program’s later directors. “I came in as a student when they expanded [class size] from 30 to 60 total students. Quite a jump, but when we first came in that year, they had no space for us, so the first four weeks of our training were held down in the basement of University Lutheran Church on University Avenue.”
Having graduated from UND and worked as a PA/FNP for years as the program saw other co- and interim directors come and go, Laxen was a good choice for helping the program take its next step.
“We were still a certificate program and had about 60 students,” Laxen explained. “After a year or so, I realized that, one, the push in PA education nationally was to have a master’s program, and, two, we wouldn’t be able to sustain the program as it was for long with both cohorts.”
That is to say, as the PA and FNP professions began to diverge and the CNPD assumed full management of the University’s nurse practitioner degree, the PA program needed to establish its own graduate degree for its matriculants. So Laxen and her team decided that UND’s program needed a master’s degree if it were to thrive.
Making this case was far from easy, though, because, as Laxen put it, in most disciplines training gets more specialized as students advance. But for physician assistants in the real world, community and clinical needs are often the exact opposite — the “expertise” should be broader.
“For the PA program, when we went toward the master’s, instead of coming to a point, we were spreading out,” Laxen continued. “We were asking folks to be proficient in five, six, seven areas of care — for a rural community.”
The dean of the SMHS at the time, H. David Wilson, agreed and helped Laxen convince the University and the State Board of Higher Education not only that a PA master’s degree was a necessary addition to the University’s repertoire, but that it should continue to be housed in the SMHS.
By 2003, the degree was official.
“Wilson supported us 110 percent,” Laxen said, adding that after Wilson, Dean Joshua Wynne has also been a staunch ally. “Some would say that [Wilson] bent over backwards to assist us when he could. We presented to the State Board, and that was just a formality. We had our ducks in a row and had the data they wanted, so we became a Master of PA Studies.”
In so doing, Laxen and crew continued the tradition Eelkema started by being an innovative, national leader in the training of what used to be called the “mid-level” provider practicing under physician supervision, paving the way for other states’ programs and developing productive relationships with a variety of cohorts, including UND’s Indians Into Medicine program.
“Whenever we went to the annual PA meetings, we were always an outlier — no one else did it the way we did, except maybe the University of Washington [Seattle],” Laxen said. “We were the only PA program whose students came from the entire U.S. All others were regional. When I was ready to retire, I figured I’d taken the program to the next step and had expanded our cadre of students beyond nurses and hired non-PAs for both lab and physiology [instruction].”

Why Not a Paramedic or Respiratory Therapist?
That trailblazing tradition and do-it-yourself ethos have only continued, suggested Rhonda McDaniel, an administrative assistant who has been with the program for 32 years.
“We were also one of the first programs to teach online,” she chimed. “And our average student age was 42 years for a long time. The national group always thought we had an error when we reported the data [on incoming students’ years of health care experience], and we’d say, ‘No, they do have 20-plus years of experience compared to these other programs.’”
The reason for this is that the program has had both to fight to make room for itself — in the clinic and classroom — and find ways to advance its profession despite limited resources and a fluid health care environment. As such, it had for years taken in only the most experienced students with strong health care backgrounds.
But as times changed, so did the now UND Department of Physician Assistant Studies.
“In 2006, we expanded our admissions process to consider applicants who were not nurses,” added Jeanie McHugo, a South Dakota native who came to UND in 2004.
“We started to track different calls we’d get from applicants who weren’t nurses, and asked, ‘Well, why wouldn’t a respiratory therapist or paramedic make a good PA?’”
After an admissions retreat and much discussion and research, the PA team decided to enroll a pilot group of non-nurse applicants. The pilot was successful, said McHugo, so the department adopted the new enrollment procedure.
And then, now with McHugo at the helm, the program started fielding queries from younger prospective students with strong backgrounds in biological science and health, but less advanced clinical experience. These applicants typically come from rural communities in the region and are interested in serving those communities after graduating.
“There was a time when a UND biology grad with a strong health interest couldn’t apply to our program,” McHugo continued. “So, we tried a pilot of these students, those extremely strong in science but not formally licensed in an advanced health profession.”
And this group too has performed just fine in both its preclinical and clinical work, according to McHugo. In fact, a recent comparison of scores between SMHS students with clinical backgrounds and those without showed that the “science” applicants perform slightly better in the basic sciences portion of the PA curriculum — and are comparable in the clinical setting.
“It’s not a statistically significant difference,” McHugo cautioned, “but we’re finding that whether they’re a student who has a science upbringing or a more advanced clinical experience, if you pick the right applicant, they’ll be successful. That philosophy seems to be working well for us.”
Into the Future
So it is that today, 50 years after starting, the program offers a hybrid of online coursework combined with alternating classroom and clinical experiences — for students of all educational and professional backgrounds. The distance program provides students with the potential to complete online coursework and clinical experiences in their home, and often rural, community.
And the innovations keep coming.
“It is going in ways we never thought possible — now they can practice without a physician,” added Laxen of the recent change in North Dakota law allowing licensed PAs to practice independent of medical doctors in certain contexts. “North Dakota is one of the few states that has taken that step.”
The ongoing COVID-19 pandemic has likewise forced the program to adapt and innovate, primarily in the direction of virtual teaching and learning.
“When I came in 2004, students were postal mailing their assignments to us,” McHugo laughed. “We’d correct those and mail them back. Then they sent us assignments as an email attachment!
“Since then, I’ve had to learn between eight and 10 different platforms to deliver content. That’s an innovation we’ve had through this distance aspect. Students don’t have to physically be here for two years, as with other schools. Our program has and will continue to be advanced in terms of technology use and content delivery.”
Or, as Laxen summarized how and why UND’s PA program has continued to flourish, if you focus on relationship building and timing things just right — even during a pandemic — you’re likely to win out.
“It’s not always that your idea isn’t good — sometimes it’s the timing,” she said. “And politics is important. I don’t believe in wheeling and dealing, but I believe in not burning bridges and bringing out the positive in people.”
UND’s pioneering Department of Physician Assistant Studies hopes to be doing just that for another 50 years.
This story originally appeared in North Dakota Medicine.

About the author
Brian James Schill is the assistant director of the Office of Alumni and Community Relations at the University of North Dakota School of Medicine & Health Sciences.


