From the Dean: Match Day results
As I mentioned in last week’s column, last Friday was Match Day for our graduating medical students. The vast majority of them matched in a residency that they will start after graduation, and in which they will learn their chosen specialty over the next three to five years. Most matched with their first choice or one of their top choices, and the list of the programs at which they matched is impressive indeed. Students matched with every one of our in-state residency programs and some prestigious out-of-state programs, including those at the universities of Washington, Minnesota, Nebraska, Michigan, Iowa, California (San Francisco), and Duke University. As has been the case for quite some time, the most popular residency choice for our students is in family medicine, where we had about twice as many students selecting this field as would be expected from recent national data. We have used that metric – at least twice the national average of the percent of the graduating class going into family medicine – as a test of how well we are doing in our mission of educating primary care providers focused on rural care delivery. We monitor our progress in this regard yearly and report our success in our annual Vital Signs community report released every November.
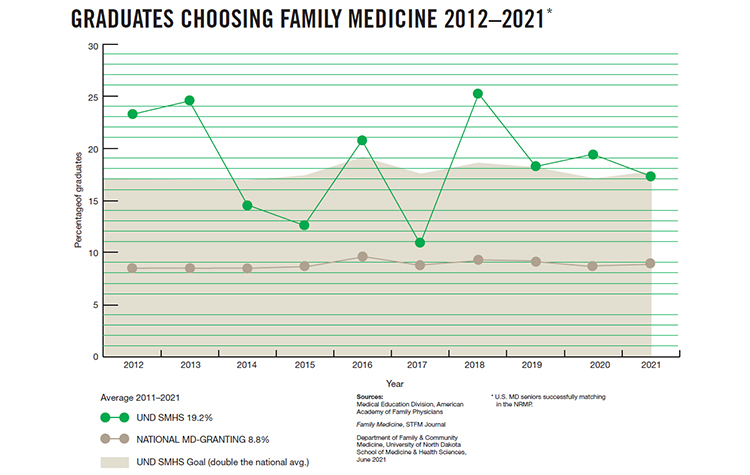 As you can see per the attached chart from the latest version of Vital Signs for 2021 (2022 data not included), for most years we meet or exceed our goal.
As you can see per the attached chart from the latest version of Vital Signs for 2021 (2022 data not included), for most years we meet or exceed our goal.
In keeping with the primary care theme, the next most popular specialty was internal medicine (although it should be noted that many students who do an internal medicine residency subsequently do sub-specialty training).
I’m especially pleased that the third most popular residency this year is psychiatry, where we again almost doubled the expected number of students who might go into the field based on national trends and statistics. This is especially noteworthy and commendable given the national awakening to the challenges and burden of substance abuse and mental health issues that have been exacerbated by the pandemic. This is good news for our fellow citizens and patients!
I’m also pleased that in both of those specialties – family medicine and psychiatry – just under half the students choosing those specialties matched with one of our in-state programs. This is important from a retention standpoint – we know that more than two-thirds of students who graduate from UND SMHS and do an in-state residency end up practicing in North Dakota thereafter. Even more, most of these physicians who return “home” to practice become clinical faculty for the School and give back to the state and School by training the next generations of physicians for North Dakota.
That’s good news for the state – and good for the students, many of whom who have family in the area. But North Dakota can only support selected residencies, as the more specialized ones aren’t feasible in a state with a population of about 760,000 people. Students interested in (for example) pathology, anesthesiology, radiology, urology, plastic surgery, or thoracic surgery of necessity must go out-of-state for training. We sure hope that after their training is completed that they’ll return home to set up their practice, and many do.
I’m sure that you’ll join me in wishing our graduating medical students all the best in the exciting future that awaits them. Congratulations to all!
Joshua Wynne, MD, MBA, MPH
Vice President for Health Affairs, UND
Dean, UND School of Medicine & Health Sciences


