National conference spotlights UND’s rural-health leadership
National conference features Cabinet speaker, draws on UND’s reputation as hub of rural health training, information, ideas

UND’s national leadership in rural health may not fill arenas, the way the men’s hockey team does.
But it does attract attention from the top people in the field – including, as recently as last month, a member of President Biden’s Cabinet.
Secretary of Agriculture Tom Vilsack was the keynote speaker at the Rural Health Journalism Workshop 2021, a virtual conference that was hosted in June by UND and the Center for Rural Health.
The three-day conference was organized by the Association of Health Care Journalists. The association – an independent, nonprofit group – boasts more than 1,500 members and is dedicated to improving “the quality, accuracy and visibility of health care reporting, writing and editing,” the association’s website notes.
And as the website continues, last week’s workshop was meant to “bring journalists together with health care and policy experts who focus on the medical needs, and how they differ, in rural areas.” That made the workshop a natural for UND and the Center for Rural Health to sponsor, said Shawnda Schroeder, Associate Director of Research and Evaluation at the Center for Rural Health, and Research Associate Professor at the UND School of Medicine & Health Sciences.
“Dr. Kay Miller, who is both a member of the Association of Health Care Journalists and an employee of the Rural Health Information Hub here at the Center for Rural Health, connected the Association with UND to see about our interest in hosting and sponsoring the conference,” Schroeder said.
“As part of the Rural Health and Communities Grand Challenge at UND, we were thrilled to support this meeting, as well as to provide key topics and speakers for the agenda. I was very excited to attend as well as to be a speaker for one of the sessions, and I learned a great deal from all of those who presented.”

Rural recovery challenges
The conference offered seminars on rural America’s COVID response, how the federal government’s American Rescue Plan – the COVID response signed by President Biden earlier this year – has impacted rural America, and the rural health care workforce, among other topics. Some highlights from a few of the sessions:
• More than half of American lived in rural areas a hundred years ago. Today, just 19 percent are rural, many of them in the Midwest. And many of them are aging.
That was the starting point for the conference’s session on “Aging in post-pandemic rural America,” moderated by Liz Seegert of the Association of Health Care Journalists.
The trend toward a more urban population exacerbates health inequities, said Carol Myers, professor of the University of Tennessee College of Nursing in Knoxville.
“The poverty rate is higher, there is negative employment growth, and fewer working-age people in rural communities,” Myers said. “That leaves people behind.”
Moreover, those left behind when younger residents move to urban areas tend to be older, sicker, and poorer, with less access to health care and transportation, Myers continued.
“Health equity and economic vitality are intertwined,” she said. “The most significant driver of health is tobacco use, diet and exercise, and alcohol and drug use. But the choices you make are sometimes based on the choices you have. Not everyone has choices.”
Hospital and nursing home closures nationwide, along with less access to services such as Meals on Wheels, have also affected rural areas, said Carrie Henning-Smith, the session’s other speaker. Henning Smith is deputy director of the University of Minnesota’s Rural Health Research Center.
But despite those issues, there are bright spots when it comes to aging in rural America, Henning-Smith said.
Rural residents are more likely to own their homes, have better air and water quality, tend to have insurance, and have more friends and social contacts than older people in urban areas.
“Most rural residents want to age in place,” Henning Smith said. She added that more services, access to broadband, and making communities more attractive to health care providers can help that happen.
The challenge of COVID-19
• Independently from the challenges large cities experienced in the face of the coronavirus pandemic, rural areas waged their own battle with the virus, speakers pointed out at the session titled, “Rural COVID-19 response: From hospitalizations to vaccinations.”
Overall, rural counties — which are disproportionately populated by older residents – have been more susceptible to COVID, said Mark Holmes, director of the Cecil G. Sheps Center for Health Services Research at the University of North Carolina.
Since the start of the pandemic, about a quarter of hospitalized rural patients have had COVID, compared to a fifth in cities. And as of June 1, the cumulative COVID deaths per capita are nearly 30 percent higher in rural areas than in the nation’s cities, Holmes said.
These bleak statistics also follow a different time horizon in rural areas, which were initially less impacted as the virus first spread in coastal cities. Today, while cities are reopening, rural counties continue to grapple with a relatively high number of viral infections.
Furthermore, as challenging as it has been, the pandemic has only exacerbated the many problems – both economic and social – that are faced by rural hospitals, Holmes and others noted. Plagued by financial hardships, roughly 150 rural hospitals (out of about 1,800 in the U.S.) have shuttered in the last decade.
Many of those hospitals are in the Southeast, where they tended to serve predominantly Black and Hispanic populations.
As Secretary Vilsack further explained in his keynote address, Congress in recent months has provided billions of dollars to keep rural hospitals open as the hosptials serve a vial role in treating COVID patients and increasing the vaccination rate nationwide.
Defining ‘rural’
• How are rural areas defined by various federal agencies, and how do these definitions square with practical reality of covering rural health issues?
Moderated by Melissa Patrick, a reporter for Kentucky Health News, the panel discussion titled “Defining rural health and rural residents” sought to help journalists covering rural health news apply information in ways that impact rural residents.
Steven Hirsch, a public health analyst with the Federal Office of Rural Health Policy, explained how various federal agencies define “rural.”
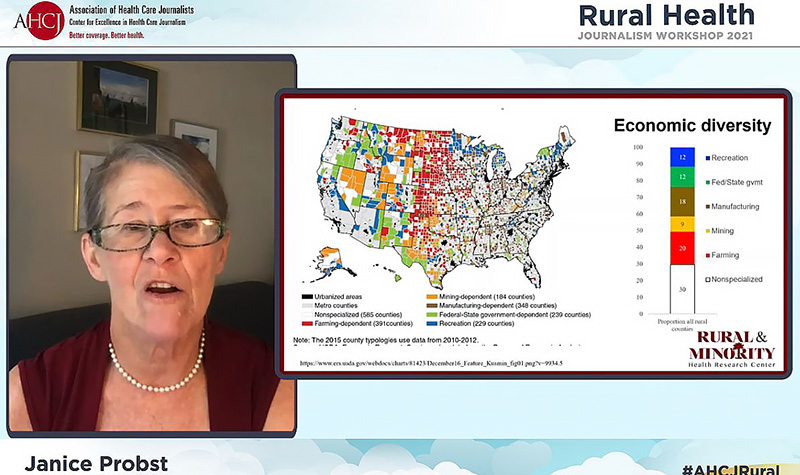
Janice Probst, director emerita with the Rural and Minority Health Research Center at the University of South Carolina, sought to bust myths about rural America through the use of data from a variety of sources. For example, contrary to the idea that rural areas are largely white and dominated by agriculture, 20 percent of the population is non-white, and mining and manufacturing represent large segments of rural economies.
Trudy Lieberman, a contributing editor with the Center for Health Journalism, discussed her experience with successfully using digital journalism to provide residents of rural states with healthcare policy information. She said the desire for useful information on such issues as hospital safety and end-of-life care transcended the perceived political persuasions of most rural populations.

Rural mental health care
• “So I was working with one lady from our National Alliance for Mental Illness chapter here in Arkansas, and she said, ‘You know, mental illness is the only illness here in Arkansas where you don’t get a casserole when you have it.” Thus spoke Tiffany Haynes, co-director of the Translational Research Institute at the University of Arkansas for Medical Sciences, during the workshop’s conference titled, “Barriers and innovations in rural mental health care.”
As Haynes suggested, mental illness often carries a stigma in rural America, and that’s just one of many barriers that can prevent people from getting treatment.
The shortage of behavioral health providers is another; there are 574 federally recognized American Indian tribes, but the Society of Indian Psychologists counts only a few hundred members, said Jacqueline Gray, associate director for Indigenous programs at UND’s Center for Rural Health.
Then there’s the bias in funding agencies against culturally relevant treatments, such as the equine assisted therapy that draws upon the Native culture of the horse, and the canoe therapy employed by some Washington and Oregon tribes.
“These are all things that have been integrated into various treatments with great success,” Gray said. “But they don’t fit into ‘evidence-based practices.’ Instead, this is “practice-based evidence,’ and the practices have been going on for thousands of years.”
Teletherapy and improving mental-health literacy are among the realistic solutions that can help lower the barriers of accessibility and stigma, respectively, speakers at the session agreed.



